Shin splints are a common and often frustrating overuse injury that affect many active Australians. Characterised by pain along the inner, lower portion of the shin, shin splints can range from a dull ache during exercise to a severe, throbbing pain that persists long after activity has stopped. At ModPod Podiatry, our Sydney podiatrists — with clinics in Dee Why, Mosman, Rose Bay, North Ryde, and the CBD — see and treat shin splints regularly, helping athletes and everyday patients get back on their feet faster.
What Are Shin Splints?
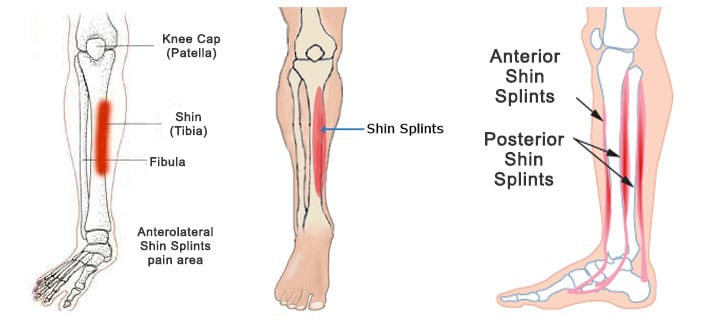
The term “shin splints” refers to pain along the tibia (shinbone), most commonly felt along the inner edge. Medically, the condition is known as medial tibial stress syndrome (MTSS). While “shin splints” is a general term, it usually describes one of the following underlying issues:
- Micro-tears in the shin muscles from overuse
- Inflammation of the periosteum (the membrane covering the tibia)
- Inflammation of the muscles and tendons surrounding the shinbone
Pain is typically felt over an area of at least 5 centimetres and often affects both legs, though it may predominantly affect the dominant leg. It is usually felt during or after physical activity, particularly high-impact exercise.
Who Gets Shin Splints?
Shin splints are particularly common among:
- Runners — especially those who have recently increased their training load or started running on harder surfaces
- Dancers — due to the repetitive impact and footwork involved
- Military recruits — who undergo intensive physical training programs
- Team sport athletes — in sports like soccer, netball, basketball, and AFL
In Sydney’s active population, shin splints are one of the most frequent complaints we see at ModPod Podiatry — particularly among runners training for events like the City2Surf or half-marathons.
Common Causes of Shin Splints
Although the exact cause of shin splints is not always clear-cut, several risk factors are well established:
- Sudden increases in training intensity or volume — the most common contributing factor
- Running on hard or uneven surfaces — increases impact forces through the lower leg
- Worn-out or poorly supportive footwear — reduces shock absorption
- Flat feet or overpronation — alters lower limb mechanics and increases stress on the tibia
- High-arched rigid feet — reduces the foot’s ability to absorb impact
- Muscle weakness or tightness — particularly in the calves, hip flexors, and core
- Being overweight — increases the load on the lower limb with each step
Symptoms of Shin Splints
Shin splint symptoms can vary depending on the stage of the condition:
- Dull, aching pain along the inner aspect of the shin
- Pain that worsens during or after exercise and may ease with rest in early stages
- Tenderness to touch along the tibial border
- Mild swelling of the lower leg
- Pain that starts at the beginning of a run, eases during exercise, then returns afterwards
- In more advanced cases, pain that persists even at rest
Shin Splints vs. Stress Fractures: What’s the Difference?
It is important to differentiate between shin splints and a tibial stress fracture, as both cause shin pain but require different management. A stress fracture causes more localised pain (often pinpoint tenderness over one spot), is almost always unilateral, and does not ease once warmed up. Shin splint pain is typically diffuse, spanning at least 5 cm along the bone.
If shin splint treatment is not followed or load management ignored, stress fractures can develop as a direct complication. A podiatrist or doctor may order an X-ray or MRI to rule out a stress fracture if symptoms are severe or not improving.
Treatment for Shin Splints
The good news is that most shin splint cases resolve well with the right treatment. At ModPod Podiatry, our Sydney podiatrists take a comprehensive approach:
1. Load Management and Rest
Reducing or temporarily modifying exercise is usually the first step. This does not always mean complete rest — low-impact cross-training such as swimming or cycling can help maintain fitness while the tibia recovers.
2. Footwear Assessment
Worn-out or inappropriate footwear is a major contributor to shin splints. Our podiatrists will assess your current shoes and recommend replacements suited to your foot type and activity.
3. Custom Orthotics
If overpronation or abnormal foot mechanics are contributing to your shin pain, custom orthotics can help redistribute load and reduce stress on the tibia. Many of our Sydney patients see significant improvement with orthotics combined with appropriate footwear.
4. Stretching and Strengthening
A targeted rehabilitation programme can address the muscle imbalances that predispose you to shin splints. This typically includes calf stretches, tibialis anterior strengthening, and hip stability exercises.
5. Graduated Return to Activity
Returning to running too quickly is the most common reason shin splints recur. A structured, progressive return-to-run programme helps rebuild capacity safely. Explore our article on 5 effective treatments for shin splints for more detail.
Frequently Asked Questions About Shin Splints
How long do shin splints take to heal?
With appropriate management, most cases of shin splints improve within 2–8 weeks. More severe or chronic cases may take 3–6 months to fully resolve. The key is reducing load early and addressing the underlying cause, rather than pushing through the pain.
Should I stop running if I have shin splints?
Not necessarily, but you should significantly reduce your training load. Running through severe shin splint pain risks progressing to a stress fracture, which requires much longer recovery. A podiatrist can help you modify your training to allow healing while maintaining fitness.
Can flat feet cause shin splints?
Yes. Flat feet or overpronation cause the tibia to rotate inward with each step, placing increased stress on the shin muscles and bone. This is one of the most common biomechanical contributors to shin splints. Custom orthotics can significantly reduce this load and help prevent recurrence.
Are shin splints the same as a stress fracture?
No, though they are related. Shin splints involve inflammation of the muscles and periosteum surrounding the tibia. A stress fracture is an actual crack in the tibial bone. Both are overuse injuries, and shin splints can progress to a stress fracture if left untreated. A podiatrist or doctor can help differentiate between the two.
Do orthotics help with shin splints?
Yes, for many patients. Custom orthotics help correct biomechanical factors such as overpronation that increase stress on the tibia. When combined with appropriate footwear and a graduated return-to-activity programme, orthotics can be very effective in preventing shin splints from returning.
Can a podiatrist treat shin splints?
Absolutely. Podiatrists specialise in the biomechanics of the lower limb and are well-placed to assess and treat shin splints. At ModPod Podiatry in Sydney, our podiatrists will assess your gait, footwear, and training habits to identify contributing factors and create a personalised treatment and prevention plan.
Book a Shin Splints Assessment at ModPod Podiatry Sydney
If you’re struggling with shin splint pain, early intervention is the best way to prevent a minor issue from becoming a major setback. Our experienced Sydney podiatrists at ModPod Podiatry provide thorough assessments and evidence-based treatment to get you back to the activities you love.
With clinics in Dee Why, Mosman, Rose Bay, North Ryde, and the CBD on Hunter Street, we’re conveniently located across Sydney. Book your appointment online today or call (02) 9960 3981.


