Fungal Nail Treatment in Sydney
If your toenails are thick, yellow, or crumbling — you most likely have a fungal nail infection. It will not clear up on its own. The longer you wait, the deeper the infection grows and the harder it becomes to treat.
At ModPod Podiatry, we treat fungal nails at five clinics across Sydney. We test first, then match you with the right treatment based on how far the infection has progressed. No guesswork. No one-size-fits-all approach.
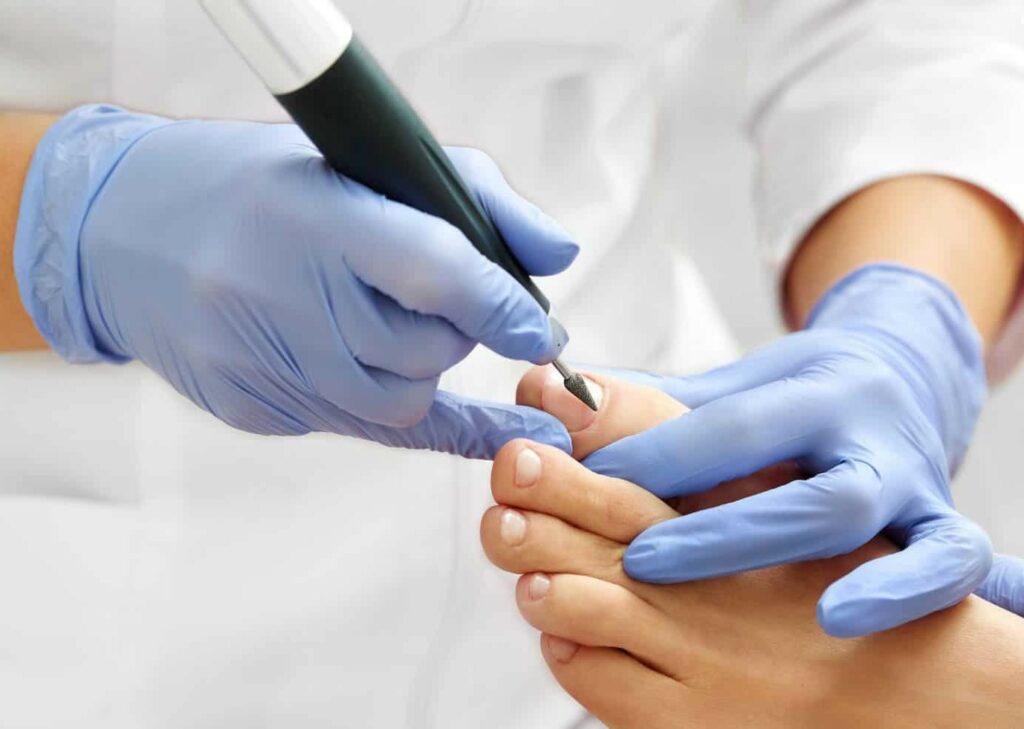
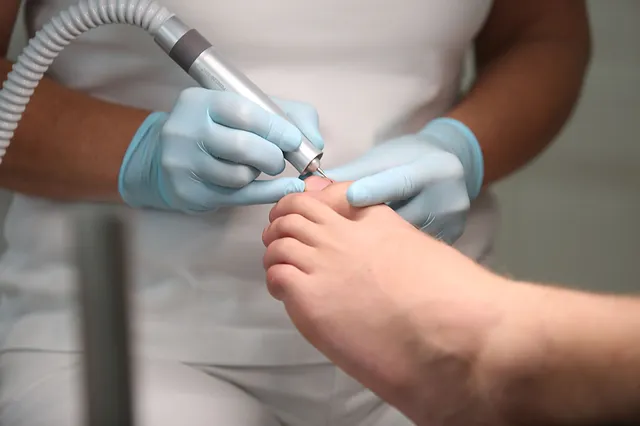
If your toenails are thick, yellow, or crumbling — you most likely have a fungal nail infection. It will not clear up on its own. The longer you wait, the deeper the infection grows and the harder it becomes to treat.
At ModPod Podiatry, we treat fungal nails at five clinics across Sydney. We test first, then match you with the right treatment based on how far the infection has progressed. No guesswork. No one-size-fits-all approach.
How To Tell If You Have
A Fungal Infection?
Fungal nail infections (onychomycosis) affect around 10% of adults. They are more common in people over 40, those with diabetes, and anyone who spends time in warm, damp environments like pools or gym showers.
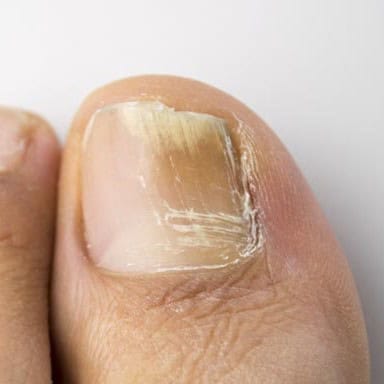
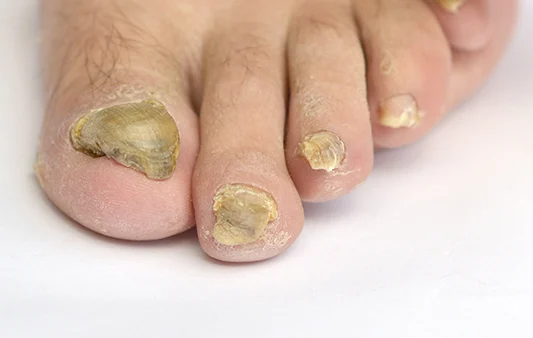
Common signs:
– Yellow, white, or brown discolouration
– Thickened or raised nails
– Crumbly or brittle edges
– Nail separating from the nail bed
– A foul smell
These symptoms can also be caused by nail trauma, psoriasis, or ageing. That is why it is worth an assessment.
Not sure what you’re dealing with? Use our free AI Nail Scanner — scan your nails with your phone camera and get a result in 60 seconds.
How We Diagnose Fungal Nails
We use visual diagnosis. At your first appointment, your podiatrist will:
1. Examine your nails under proper lighting and magnification
2. Review your medical history and any previous treatments
3. Assess the pattern, colour, and texture changes to identify the infection type
We do not rely on nail clippings. Lab cultures take weeks to return results and produce a high rate of false negatives. Visual diagnosis by an experienced podiatrist is faster, more reliable, and means you start treatment at your first visit — not weeks later.
Your Treatment Options
There is no single “best” treatment for every patient. The right option depends on how many nails are affected, how severe the infection is, and your medical history. Here is what we offer:
Cold Laser Therapy (Lunula Laser)
Our primary treatment. The Erchonia Lunula Laser uses two wavelengths of light to target the fungal cells and boost your body’s immune response. There is no heat, no pain, and no side effects.
- Sessions: 4–8 weekly, around 12 minutes each
- Suitable for mild, moderate, and severe infections
- FDA cleared for treating onychomycosis
ModPod was the first practice in Australia to use this technology. We have treated over 10,000 patients with it.

Topical Antifungal Therapy
Prescription-strength antifungal lacquers applied to the nail surface. Used on their own for mild infections, or alongside laser for moderate to severe cases.
– Cure rate: 5–17% on their own; higher when combined with laser
– Duration: Daily application for 6–12 months
– No systemic side effects
Combination Therapy
Evidence shows that pairing laser with topical antifungals gives the best results. The laser clears the deeper infection while the topical prevents reinfection at the surface.
Your podiatrist will recommend the right combination based on your test results.
Want to compare all treatment options in detail — including oral medication and home remedies? Read our full breakdown:
Why Patients Choose Modpod

Expert Podiatrist Assessment
Your podiatrist examines your nails under magnification, reviews your history, and identifies the infection type at your first visit.

10,000+ Patients Treated
We were the first practice in Australia to use the Lunula cold laser for fungal nails. We have more experience with this technology than any other clinic in Sydney.

AI Nail Scanner
Our free online tool lets you scan your nails at home before you even book an appointment. It gives you a quick indication of whether your nails may be fungal.
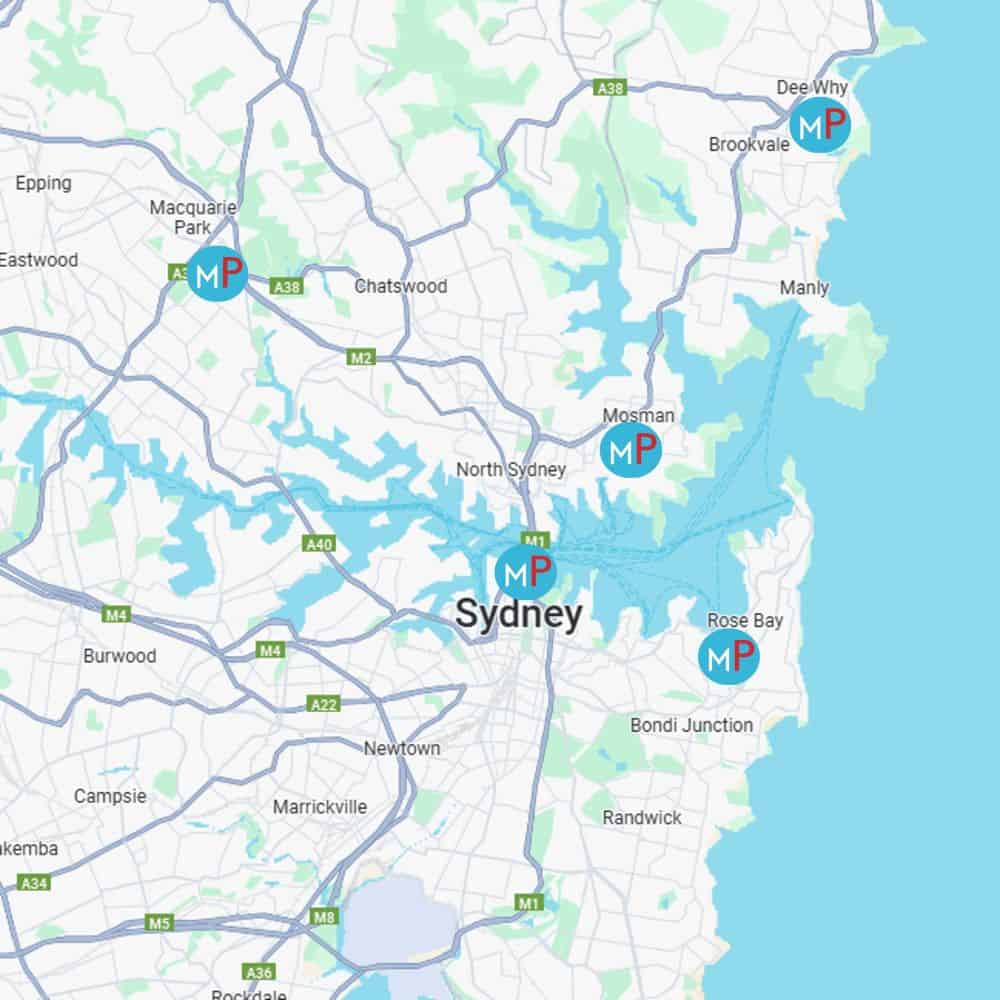
Five Sydney Clinics
Treatment is available across all our locations — choose the clinic closest to you.

Combination Approach
We do not rely on one treatment alone. We match the approach to your infection, which is why our results are consistent.

Preventative Care Program
Once you have undergone treatment your podiatrist with give you a tailored post treatment plan to prevent reinfections.
What Happens If You Do Not Treat It
Fungal nail infections do not resolve on their own. Without treatment:
- The infection can spread deeper into the nail
- It can spread to other toenails
- It can spread to the skin around the nail (athlete’s foot)
- The nail may become painful or difficult to trim
- In people with diabetes or poor circulation, untreated fungal nails increase the risk of secondary infection
Early treatment gives the best chance of a full cure with fewer sessions.
Our Sydney Clinics
We prescribe custom orthotics at all 5 Sydney Modpod locations:
Each clinic uses the same 3D scanning and manufacturing process. If you need to visit different locations, your records transfer across the practice.
Frequently
Asked Questions
What is the best treatment for fungal toenails?
It depends on the severity. For most patients, cold laser therapy (Lunula laser) combined with a topical antifungal gives the best results — a 75–90% cure rate with no side effects. Your podiatrist will recommend the right approach after assessing your nails.
How do I know if my toenails are fungal?
Common signs include yellow or brown discolouration, thickened nails, and crumbly edges. However, up to 50% of abnormal nails are not fungal — trauma and psoriasis can look similar. Use our free AI Nail Scanner for a quick check, or book an assessment for a confirmed diagnosis.
Do I need a referral to see a podiatrist for fungal nails?
No. You do not need a referral to see a podiatrist in Australia. You can book directly with us online or by calling (02) 9960 3981.
How long does fungal nail treatment take?
Laser treatment involves 4 to 8 weekly sessions. After treatment, the nail takes 9 to 12 months to grow out fully and show the final result. Your podiatrist will monitor progress throughout.
Is fungal nail treatment covered by Medicare?
Laser treatment is not covered by Medicare. Some private health funds cover podiatry consultations — check with your provider. We provide receipts for claiming.
Can fungal nails spread to other people?
Yes. The fungus spreads through direct contact and shared surfaces — showers, pool decks, gym floors, and shared nail tools. Wear thongs in shared wet areas and avoid sharing clippers or nail files.